Ingrown Toenails Treatment in Thousand Oaks, CA
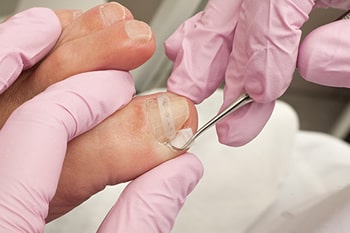
Ingrown toenails can form when the side of a toenail begins to grow into the flesh surrounding the nail. As a result, the affected toe—most commonly the big toe—may become red, swollen, painful, and—in severe cases—infected.
Causes of Ingrown Toenail
There are many reasons why an ingrown toenail may develop. Improperly cutting your toenails is a major cause of ingrown toenails. If toenails aren’t cut straight across or are cut too short, the likelihood of getting an ingrown toenail may increase. Other causes include having unusually curved toenails, wearing shoes that don’t give your toes an ample amount of space, and hereditary factors. Injuring the toe by stubbing it or having an object fall on it may also lead to ingrown toenails. If left untreated, an ingrown toenail can lead to further complications with the foot.
Ingrown Toenail Complications
If you are someone who has diabetes, it’s extremely important to remain mindful of ingrown toenail prevention, as minor cuts or simple scrapes can lead to serious complications. You can prevent ingrown toenails by ensuring toenails are straight across and at a moderate length, wearing shoes that fit properly, and checking feet daily for signs of foot issues.
Treatment for an ingrown toenail will vary on a case by case basis. One form of treatment requires lifting the ingrown nail and placing a splint or piece of cotton underneath. Another method for a more severe case would involve partially removing the nail. For cases that need extreme care, the nail itself and tissue would have to be removed.
If you’d like more information about ingrown toenails, we recommend you consult with a podiatrist who can give you a proper diagnosis and go over your treatment options.
A Patient’s Guide to Ingrown Nails
We treat hundreds (probably thousands) of ingrown nails in our office each year. Ingrown nails come in two varieties: the infected version usually found in teens and young adults and the chronic kind found in more mature patients. What they both have in common is the edge of the nail pushing against the side of the toe.
In the chronic, non-infected version, the skin is not broken. In the acute type, the nail actually penetrates the skin, causing a reaction by the body to get rid of the nail and, sometimes, an actual infection.
The traditional thought is that the nail is too wide for the toe. This might not have mattered in the eons before we, as a race, started wearing shoes. But shoes, and sometimes even socks, squeeze the toe onto the nail, and pain and trouble follow.
Sports and tight shoes contribute to this scenario, and picking and jabbing at it can get it infected. But the real problem, is that some toes just do not like to be squeezed into a shoe. Call it “no-fault” ingrown nail.
Treatment of ingrown nails differs depending on the kind you have. Teenagers who develop the infected type need to have the edge of the nail gently removed from the side of the toe. This is traditionally done by first putting the toe to sleep.
This is done with a needle and syringe injection, but we try not use these words with a scared patient. Like most podiatrists, we have developed techniques for this injection that make it as painless as possible.
After removing the edge of the nail plate, the toe is dress with a topical antibiotic and we have the patient do this as well for a couple of days. Actual infections require antibiotics.
In our office, every step of this is done with autoclaved sterile instruments while other offices sometimes use instruments just soaked in a disinfectant.
We enjoy the challenge of gently talking a scared young, and sometimes not so young, patient through the procedure.
More mature patients have the other kind of ingrown nail that never looks infected but just chronically hurts with shoe pressure. Some people have lived with this pain for years, not knowing how easy it is to fix it permanently.
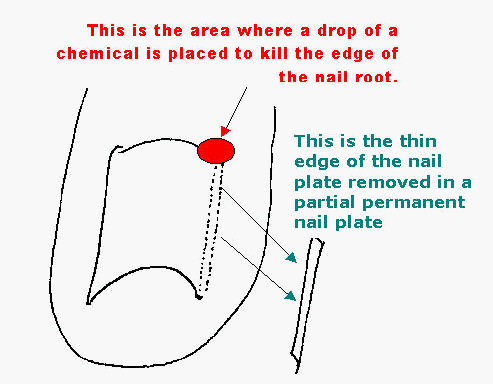
After removing the sliver edge of the nail plate, a chemical is placed by the nail root that keeps it from growing back. Recovery requires a few days of wearing an adhesive bandage.
We at ALRPC make this surgical procedure look deceptively easy. While some non-podiatrists can do this with efficiency, others are not so skilled.
When you hurt with an ingrown nail, you can nearly never go wrong going to a podiatrist who has done this so many times that his or her gentle confidence can go a long way to making what could be a frightening procedure almost a pleasure.
Every week we hear that our techniques are immensely less troubling than that which they have experienced elsewhere. The pleasure we podiatrists get doing this surgical procedure quickly, efficiently and nearly painlessly goes a long way.
The Matricectomy – A Photographic Journey
By Michael Zapf, DPM
The first photo below shows the evil ingrown nail before we started. This patient has chronic and recurrent ingrown nails on the left side of the toe (fibular border). This toe killed her in shoes. She wanted desperately to get this toe better. Others tried and others failed. Now it was my turn. The first photo below shows the painful toe. Notice that besides some redness, the toe looks normal. The offending nail border is down in the side of the toe where you cannot see. I begin by injecting the base of the toe with plain Xylocaine after first spraying the injection site with enough Ethyl Chloride (aka freezy spray) to pre-freeze the skin. I use the smallest syringe and the smallest needle made for this injection. I find these little needles and syringes produce the least amount of pain. I follow the Xylocaine injection with a second injection of long acting Marcaine. I do not start with the Marcaine because it stings so much going into the tissues that I want the toe first made numb with the gentle Xylocaine.
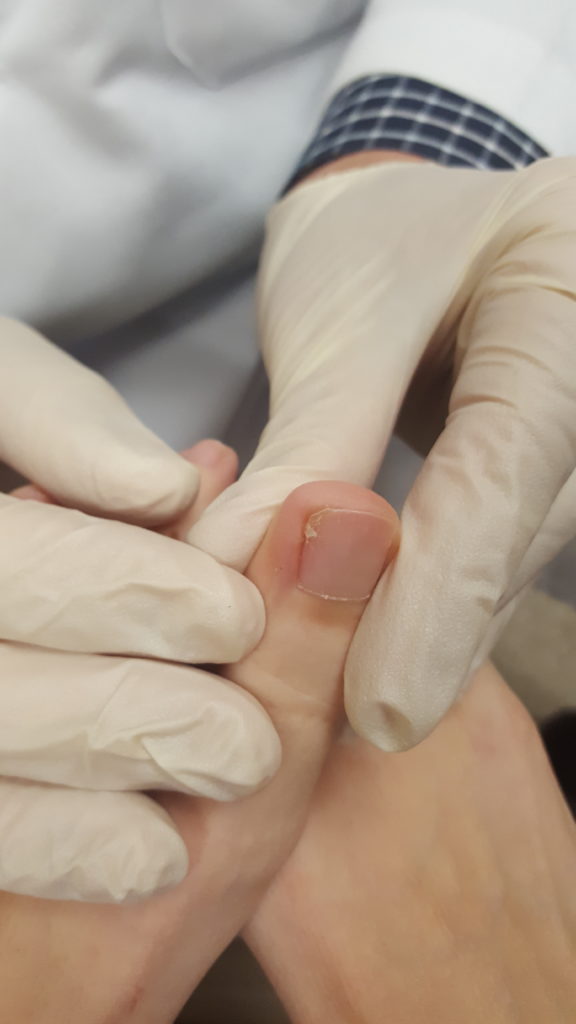
Also note that I inject at the base of the toe where the skin is loose and movable. Injecting it at the tip of the toe where it is ingrown (a favorite trick of some urgent care centers) is cruel and unusual punishment. After securing anesthesia of the toe it is scrubbed with a clear anti-bacterial solution called Clorahexidine. Next I place a blue “toe-niquet” over the toe to keep any ‘red stuff” out of the wound site. Not only do I not like the sight of the red stuff but it interferes with the effectiveness of the acid I use to kill the nail root. Next I use a tiny tool called a curette to loosen the skin away from the edge of the edge of the toe nail.
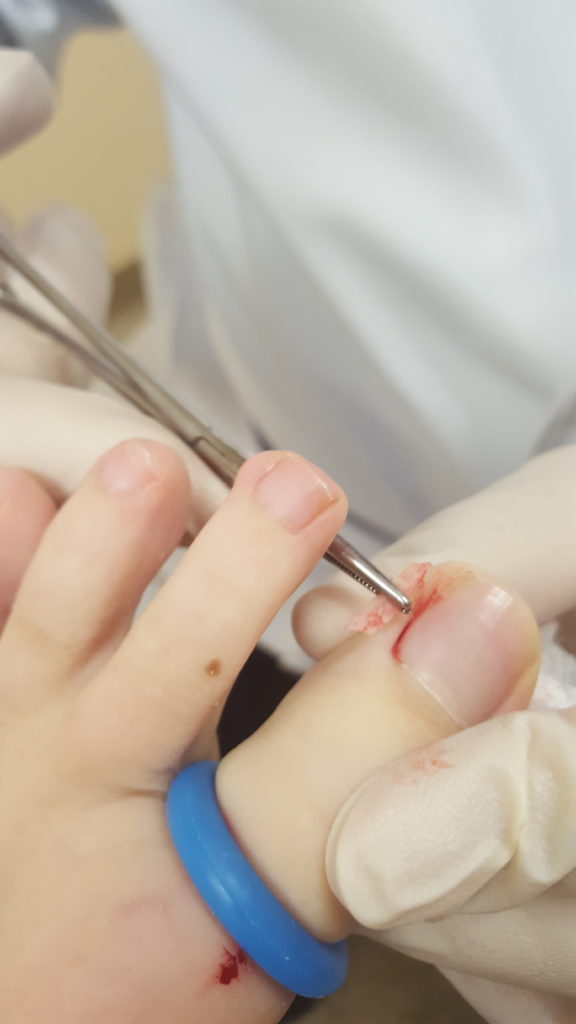
After freeing the edge of the nail plate I use an fancy nail cutter called an English Nail Splitter to cut the edge of the nail parallel to the side of the toe After cutting the side of the nail plate I use a little tweezer like instrument called a mosquito hemostat to reach in and grab the piece of nail that was inside the toe. Done correctly you do not have to remove any nail that you can see – just the nail that is inside the toe itself
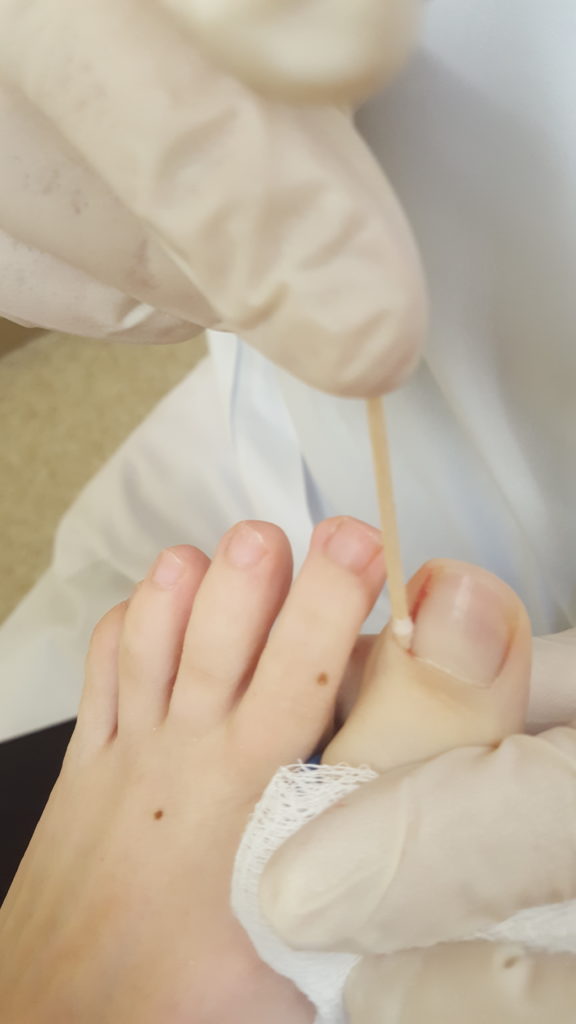
The acid being applied to the root of the nail
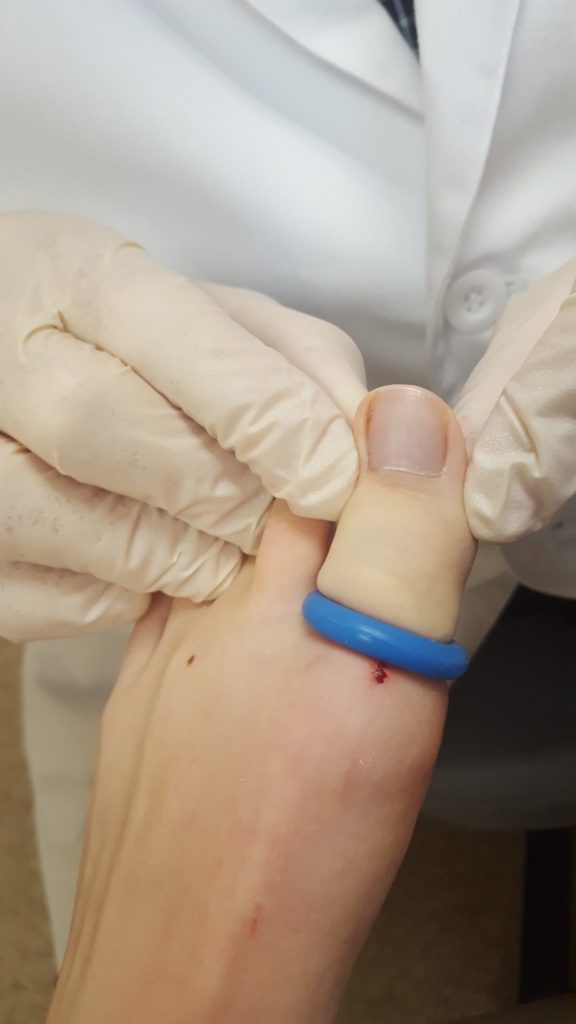
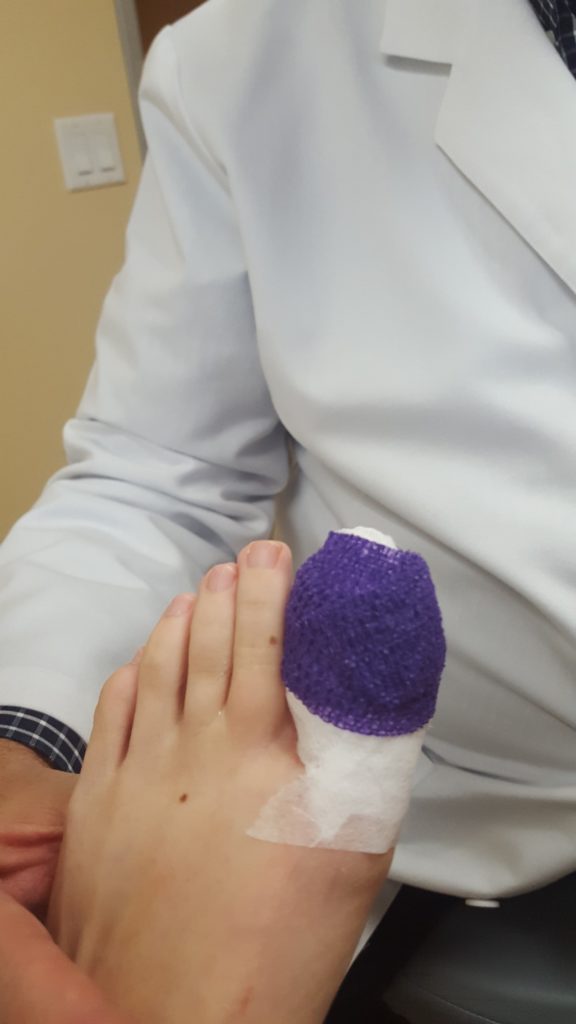
After the edge of the nail plate is removed it is time to kill the edge of the nail root that causes the edge to grow. I use an applicator stick (medical speak for a Q-Tip) that was dipped in an acid called phenol. To kill the nail root requires two or three applications of phenol placed directly on the nail root tissue. Finally the toe-niquet is removed and the toe is dressed with an antibiotic cream, sterile gauze and covered with a compressive bandage called Coban (here it is purple).
Matricectomy Post-Operative Instructions:
- It is best to return home and elevate the foot/feet until the feeling returns (which can take from 2 to 6 hours). At that time remove the stretchy Coban covering the gauze. Delay taking a shower or bath for 12 hours from the time of surgery.
- Clean the nail border(s) using any one of the three interchangeable methods (not all 3 at the same time):
- A) Using a shower of clean tap water – holding the toe(s) under the shower using it like a shower-pic.
- B) Clean the edge of the nail plate with a Q-Tip and hydrogen peroxide
- C) Soaking in an (Epsom or kitchen) salt solution and cleaning the wound edge with a Q-Tip
- Tomorrow morning do the first cleaning of the toe(s). Remove the white dressing and clean the wound(s) using one of the three methods that are interchangeable. After cleaning the nail border(s) please dress the wound with the prescription antibacterial and cover the toe with a Band-Aid. Wear regular shoes that are not too tight on the toes.
- Keep the wound clean including avoiding getting dirt or sand into he wound and showering only with a Band-Aid or other covering on the toe(s) until healing is complete. Wounds do not heal faster if they are allowed to “dry-out” or “air-out”
- Call the office if the toe becomes more swollen, painful or red than you think is normal.
- Please schedule a follow-up visit for 3 to 5 days after the procedure.
